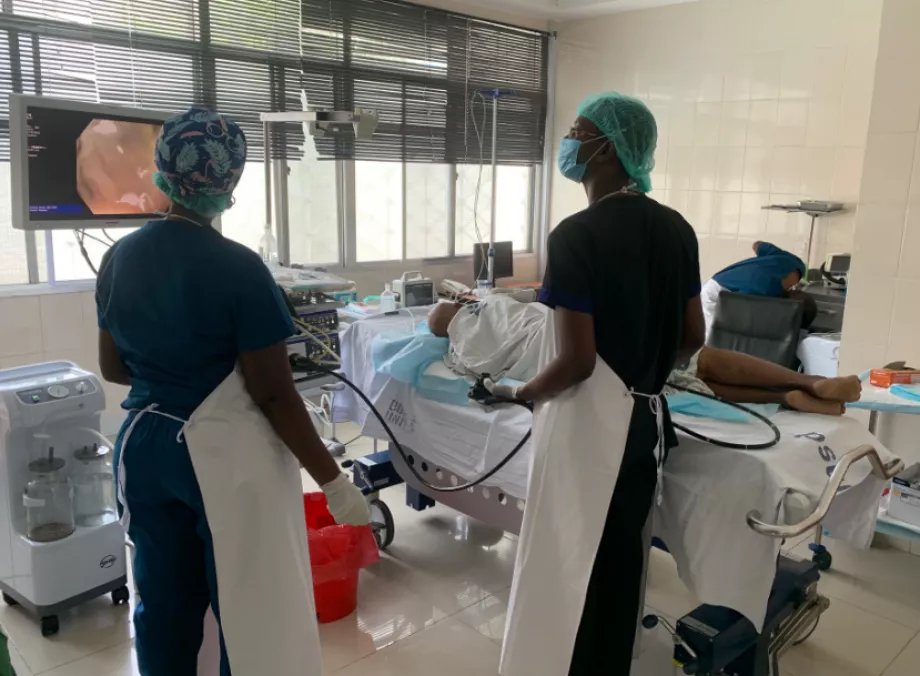
We assessed Muhimbili National Hospital as a potential WEO training center for local and regional endoscopists.
Tanzania is a rapidly developing country with many of the features we are aiming for in our training center selection. The Muhimbili National Hospital is by far the largest hospital in the country, 100% public, and seemingly outperforming the private alternatives.
Interestingly, the endoscopy unit at Muhimbili was built around 10 years ago through a generous donation brokered by the late Professor Meinhard Classen, as a joint project. Despite being a modern unit in terms of both equipment and facilities, the project never really took off until recently – with the current leadership at the hospital being very supportive of developing the endoscopy activity.
Hospital and unit
Muhimbili National Hospital is a complete public hospital with around 3000 beds. It provides most services, including a renal transplant program, a major advanced cardiac center, and also a significant orthopedic unit. The hospital also has a strong pathology service and a developing interventional radiology unit.

As mentioned, the endoscopy unit was built 10 years ago, and is similar in construction and standards to most medium-sized European units. It comprises 3 large procedure rooms, a large scope cleansing area, office space, a cooled storage room for accessories, a seminar room, and a healthy indoor patient waiting area with onsite toilets. The unit is shared by surgeons and gastroenterologists who perform procedures on 2 days each per week, with 1 day for bronchoscopy. Wifi was available in the unit, though not very functional during our visit
Equipment and maintenance
The unit has Olympus equipment with one 180 and two 190 towers. Two gastroscopes and two colonoscopes, 190 series, were presently operational, but there was also a typical graveyard of broken scopes. The unit also had a new duodenoscope, an operational C-arm for ERCP, and a recently acquired Fujifilm EUS tower and linear scope.
Scope repair frequency appears similar to other units, but the service level from the Olympus distributor in Nairobi (Nairobi X-Ray) seems quite dedicated. They also offer minor repairs (including wire tightening), and the local medical technician support also provides minor fixes – a great asset!
The unit has three Olympus trays for disinfection in addition to manual cleansing.

Staff
The endoscopy unit was staffed jointly by gastroenterology and surgery personnel. For gastroenterology, 4 consultants were all working primarily at this public hospital. Clinicians’ time is split between endoscopy, wards, and clinics. No after-hours emergency service is offered.
The surgical component of the staffing is similar. We observed friendly collaboration and splitting of resources.
The unit has 12 dedicated endoscopy nurses, who all rotate the scope cleaning. The head nurse was trained in Cairo; the group was otherwise trained onsite, apparently including repeated courses from the Olympus distributor as needed. They were competent and friendly.
There is a full anesthesiology service, one per room, offering a propofol/fentanyl combination as needed (e.g. for children and for most colonoscopies).
Training
Tanzania requires a 2-year fellowship program for gastroenterology. This does include endoscopy training, and also a compulsory completion of a research thesis, although apparently the latter is not too ambitious and there is no push for publication. For surgeons endoscopic training is not compulsory, but is offered as needed
Endoscopy activity
Thirty procedures were scheduled for the day we observed, with about equal numbers of upper GI procedures and colonoscopies. There were 4 procedures in children, and two bougie dilations. Most procedures were done by consultants.
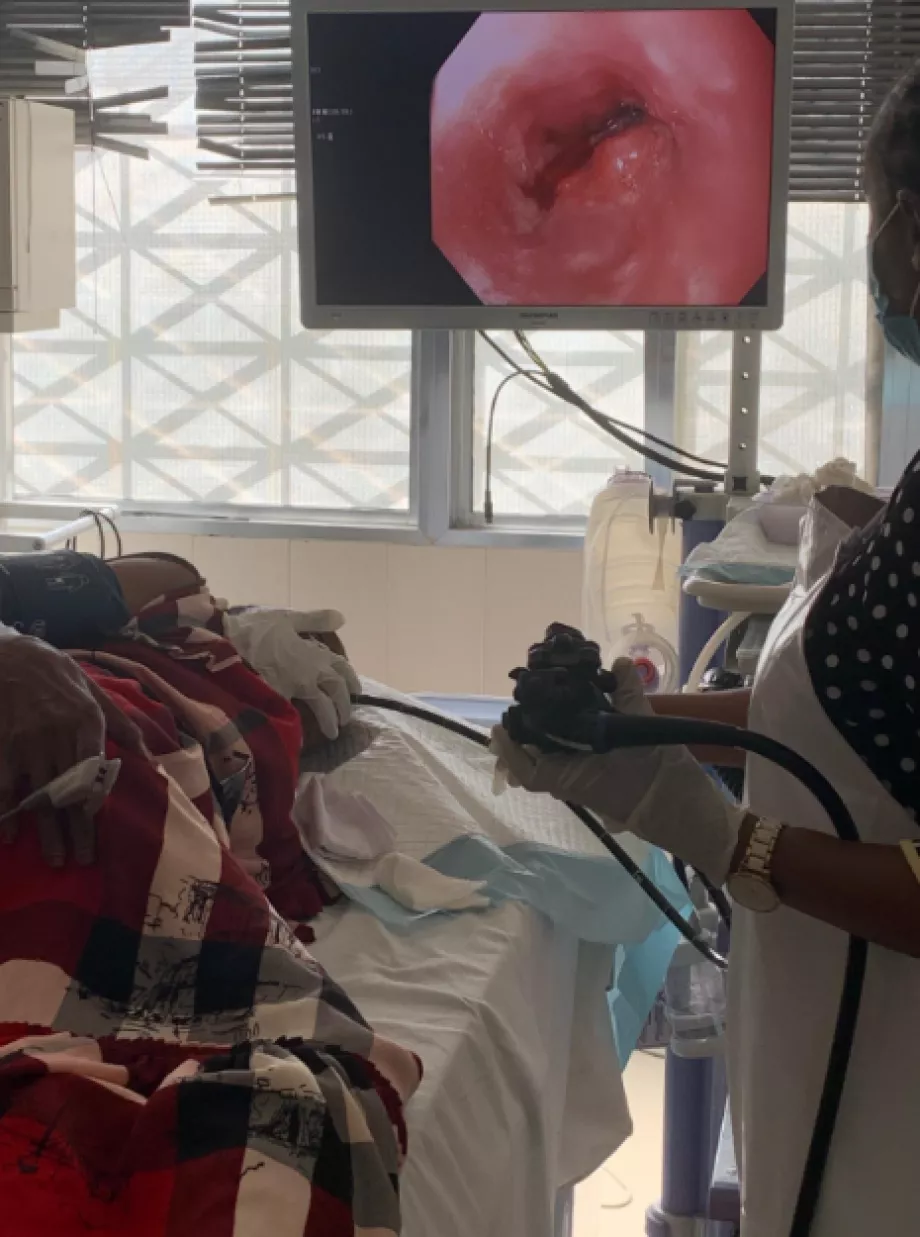
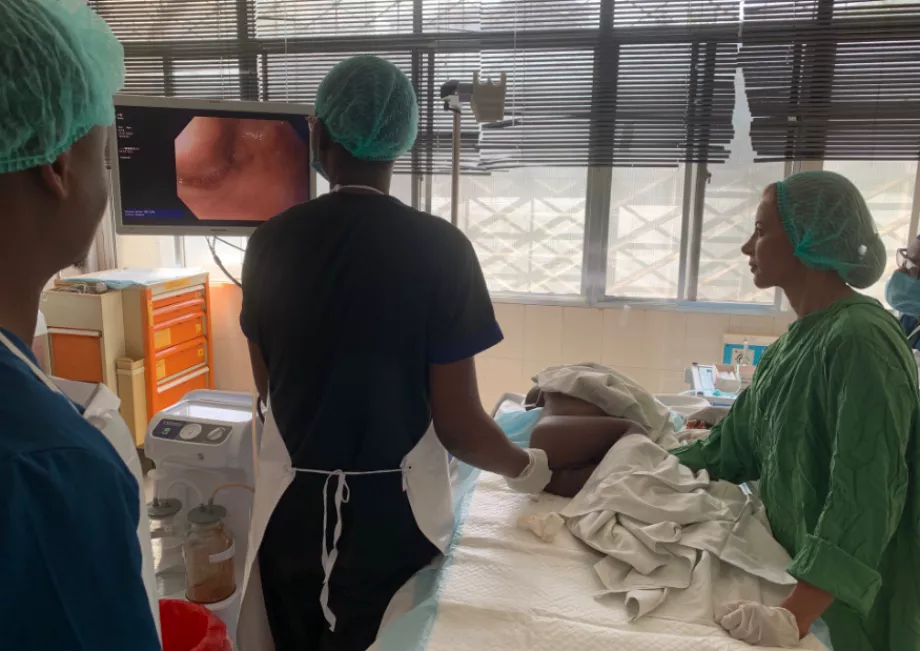
During our morning visit, (a surgeon-performed endoscopy session) we saw one gastric cancer and one esophageal cancer that were both biopsied. We also saw one large (>30 mm) pedunculated polyp in the sigmoid, which we strongly advised against removing given that no hemostatic tools or Endoloop were available. Otherwise there was a notable number of negative procedures for poor indications, which is concerning in a low-resource environment. Endoscopic technique in general was acceptable, but there was definitely room for mentoring in technical skills, particularly in colonoscopy. All procedures resulted in terminal ileum intubation, albeit with some guidance.
We know of 9 placements of esophageal stents in December, as well as band ligations, fundic varix cyanoacryl injections and removal of small polyps. Around 600 procedures are performed in total per month, the great majority diagnostic. Biopsies are taken, and brought to the pathology department by patients themselves and require additional payment, but apparently the system works satisfactorily.
There is one endoscopy nurse per procedure, and one anesthesia nurse, and anesthetist in one room.
The unit has ERCP and EUS equipment and a setup in place, including a radiation-shielded room with a C-arm within the endoscopy unit. Currently no ERCP/EUS activity takes place yet because of training issues.
Documentation
Reporting is computerized, basically template-based with very little detail but structured and connected to the hospital records. There is no facility for summary data extraction or other reports beyond the individual endoscopy report. A general ledger is kept manually, also relatively undetailed (but including procedure type etc).
Accessories and procurement
The model was somewhat similar to that in Addis Ababa, with accessories being bought as needed directly by patients at the in-house pharmacy. These included, at least, band ligators, injectors, glue, snares, and esophageal stents, but at quite high cost (e.g. 150–200 USD for a band ligator). This resulted in quite high numbers of patients who underwent an EGD in which varices were found but who were unable to afford to buy the necessary equipment for treatment. It did not seem that clips were available at Muhimbili.
Research
There was very limited activity within gastroenterology/endoscopy. There was some interest from the fellows group in initiating simple trials; we will pursue that.

Meetings
We had lengthy discussions with the leadership of the endoscopy unit about the operation of the unit. We met with the interventional radiology/HPB surgery team to discuss variants of collaborative avenues. We had a top-level talk with the director of the hospital who appeared very strongly poised to support the further development of endoscopy activity and visibility of gastroenterology at Muhimbili. Finally, we had a larger group meeting with many of the fellows from gastroenterology and surgery, discussing freely their views on issues, wishes, limiting factors, etc.
Conclusion
This visit afforded a relatively detailed examination of the endoscopy services in Muhimbili hospital in a short time. Our impression was that it was a functional endoscopic unit that would require some commitment and work to improve to international standard, but that these are highly achievable goals.
The environment is currently very favorable: the endoscopy unit and its building design and provisions for patients and staff is a big plus. The new hospital administration is receptive to the idea of change. The staff, both nurses and doctors, are motivated, dedicated, and well-trained. There is a reliable supply of consumables and at least a basic amount of equipment for moving forward. There is a strong desire to learn advanced procedures including ERCP and EUS.
We now need to find a balance between what the hospital can and should provide in terms of resources and modifications of the current setup, and what kind of training and other support can be provided by WEO. A further document outlining the details will be drafted and will form the basis of our Memorandum of Understanding with Muhimbili National Hospital.